No content results match your keyword.
Content
You have successfully logged out.
Prevention surgical site infections
Prevention of surgical site infections (SSI)
The aim of all hygiene measures is to reduce surgical site infections and other hospital-acquired infections, and to protect employees from occupational infections. In order to keep the infection rate as low as possible, you should consider and optimize the entire process and develop bundle strategies.
Focus topic
Post-operative wound infections in veterinary medicine (SSI – Surgical Site Infections).
Learn moreThe following processes should be considered for the targeted prevention of surgical site infections.

Preoperative examination of the patient/decolonization: The patient’s health status is an important risk factor for SSI.1, 2 Patients should therefore be thoroughly examined before surgery and, if necessary and possible, diseases and/or local skin infections should be diagnosed and treated before surgery.
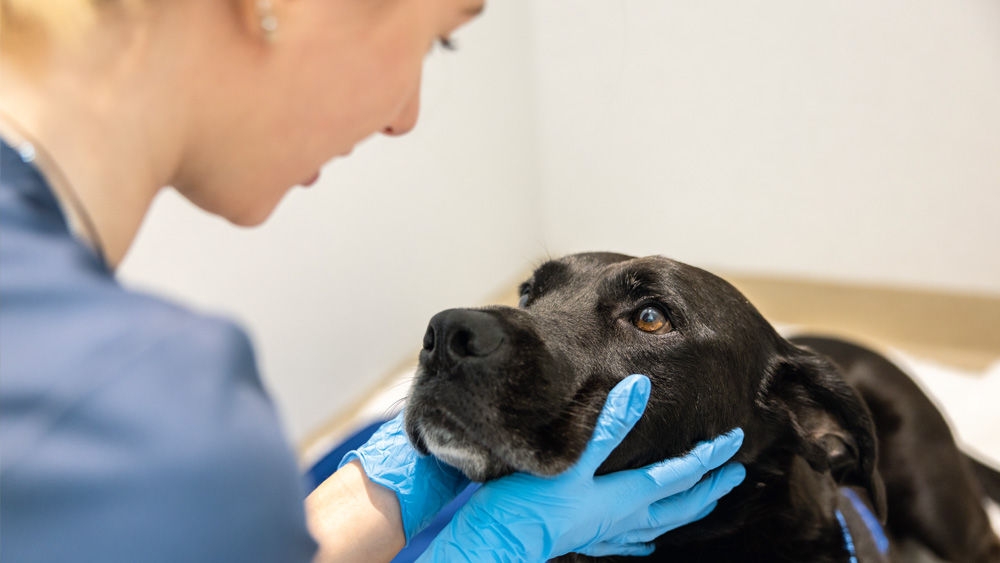
Optimization of anesthesia time: The total duration of anesthesia, as well as the total duration of the operation, has an influence on the SSI rate,2-4 and should therefore be kept as short as possible. This can be achieved through good planning of the surgery day and by optimizing general processes.
Normothermia: Perioperative hypothermia is associated with an increased SSI rate in human medicine. There is little clear evidence of this in veterinary medicine, but hypothermia is associated with an extension of the recovery phase and thus the anesthesia time,5, 6 which has a substantial effect on the SSI rate.2-4, 7 Perioperative hypothermia is also associated with an increased mortality rate in emergency procedures.8 The patient’s temperature should therefore be a component of regular monitoring to ensure that therapeutic measures can be initiated wherever necessary.
Hypotension: Animals that become hypotensive during surgery are 27 times more likely to develop a surgical site infection. Therefore, blood pressure should be monitored and, if necessary, treated throughout the anesthesia.9
Oxygenation: Hypoxia has been described as a risk factor for SSI in numerous studies in human medicine.10-12 Oxygenation should therefore be monitored and corrected, if necessary, throughout the entire operation and anesthesia time.
Glucose: Perioperative hyperglycemia is associated with an increased SSI rate.13-15 Therefore, especially in patients with diabetes mellitus, glucose should be monitored and treated if necessary16, 17 before and during the entire operation.
Preoperative hair removal: The area to be operated on must be adequately shorn over a large area (at least one hand width around the expected incision site). The hair should be cut outside the area to be operated on and as gently as possible to protect the skin (no wet shaving). Ideally, all diagnostic measures, such as X-rays, are to be carried out before the shearing. A shear immediately before surgery is recommended. There should be a maximum of 4 hours between the shear and the operation.18, 19
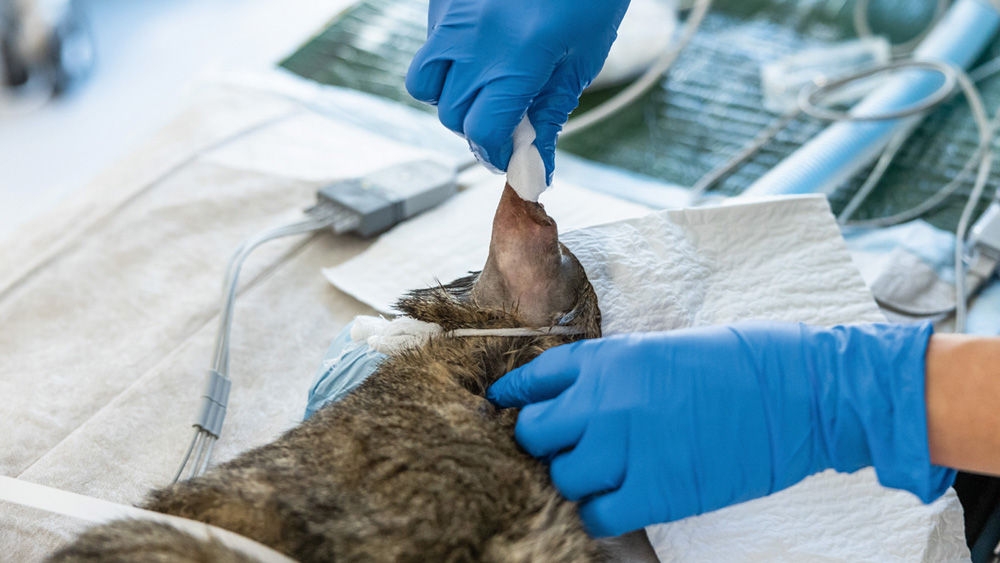
Preoperative washing: In human medicine, it is recommended that patients wash thoroughly in the evening or early morning before surgery,13, 20, 21 to achieve a significant reduction in skin flora. As this is difficult to achieve with animal patients, thorough cleaning of the operating area after shearing should be carried out. The aim is to reduce transient skin flora and to remove sebum, grease, and dirt. Water and soap should be avoided as they can reduce the effect of the antiseptic (e.g., alcohol).22 Skin can be cleaned using a dry foam or cleansing lotion. The product is applied to the shaved skin with a near-sterile compress or cloth and the skin is cleaned. After 1-2 minutes, dry off the residue with a clean cloth or swab.
If the patient is being washed at home by the owner, the patient’s coat should be thoroughly rubbed and cleaned with a washcloth soaked in cleansing solution or cleansing foam. After 3-5 minutes, rub the fur dry with a clean towel.
Antisepsis of the surgical area: Antisepsis plays a key role in the prevention of SSIs, as the transection of the skin enables the resident flora to be spread deep into the surgical area. Alcohol is the first choice due to its rapid and good efficacy.13, 20, 21 The discussion about the residual active ingredient remains controversial. Traditionally, PVP iodine or chlorhexidine is the agent of choice in some countries. Studies from human medicine have given preference to one or the other active ingredient. In a meta-analyses of the different studies, none of the two antiseptics showed any advantage over the other.21, 23 However, the effect of chlorhexidine on multi-resistant Staphylococcus aureus is reduced compared to that of PVP iodine. [24] Other authors have reported chlorhexidine resistance with Escherichia coli, Salmonella spp., Staphylococcus aureus or coagulase-negative staphylococci, Enterobacter spp., Pseudomonas spp., Proteus spp., Providencia spp. and Enterococcus spp.25
We therefore recommend the use of a PVP-iodine alcohol preparation.
The patient’s skin is rubbed for 30 seconds with a sterile swab soaked in Braunoderm® and with the aid of sterile grain forceps with Braunoderm®. Always work outwards from the expected area to be incised. Comply with the contact time specified by the manufacturer and then repeat the process 2 more times. PVC iodine (Braunol®) or polyhexanide can be considered for mucosal antisepsis.20
Incision film: Studies on the use of incision film in veterinary medicine are lacking. In human medicine, incision films that are not antiseptically impregnated are not recommended as they can increase the risk of SSI.26
In the AESCULAP® Surgical Instruments online catalog, you will also find the matching forceps and kidney trays.
Surgical scrubs: Surgical scrubs are designed to prevent bacterial spread in both directions. Although the infection prevention effect has not been demonstrated in any comparative study, this procedure appears to be advantageous, as normal workwear can become contaminated with potential pathogens, including MRPs (multi-resistant pathogens).27, 28

Surgical scrubs: Surgical scrubs are designed to prevent bacterial spread in both directions. Although the infection prevention effect has not been demonstrated in any comparative study, this procedure appears to be advantageous, as normal workwear can become contaminated with potential pathogens, including MRPs (multi-resistant pathogens).27, 28
Hair protection and surgical mask: Wearing hair protection and a surgical mask are plausible. Microbial contamination of the room air has been proven, so that both protective measures should be worn in the operating room and during the operation.29, 30
Surgical shoes and shoe covers: Bacteria introduced from outside can increase the bacterial content in the air and thus contribute to air contamination by up to 15 percent. 31, 32 It is therefore recommended to wear surgical shoes or covers.
Sterile protective clothing: Sterile protective clothing provides a barrier function that is especially important for the protection of operating room staff. Disposable gowns are significantly less permeable to bacteria than washable cotton gowns and are therefore preferable.33, 34 Single-use surgical gowns are also better from an economic perspective and can reduce the SSI rate.34-36
Safety goggles: Protective goggles should be worn during all procedures where there is a risk of splashing body fluids or potentially infectious material (e.g., septic surgery, dentistry, working with oscillating or rotating devices, granulomas).
Hand washing: Hand washing is the first step in preparing for the surgical day and should be carried out before donning surgical scrubs. If possible, there should be a gap of at least 10 minutes between hand washing and alcoholic hand disinfection, as this excludes the possibility of a reduction in the efficacy of the alcohol.22 Hand washing should also not be carried out routinely before every operation, as washing degreases the skin repeatedly, which in turn, leads to drying out and damage to the skin.20 Another hand wash should be carried out before re-entering the operating area should personnel leave the surgical tract between operations and pursue other activities. In general, hands should be washed with a perfume-free, pH-neutral soap, such as Softaskin® pure. Hand washing for 15 seconds is sufficient to significantly reduce spores, dirt and organisms.
Surgical hand disinfection: Surgical hand disinfection must be carried out by all personnel involved in the operation and also before each operation. Alcohol-based preparations, such as Promanum® pure, represent the agent of choice. The rubbing time should be at least two minutes (irrespective of the manufacturer’s specifications if under 90 seconds).37-41
Surgical gloves: Surgical gloves come in different qualities and materials. Glove perforation is a major problem during surgery. Latex gloves have been shown to be less susceptible to perforation, e.g. Vasco® OP-Grip/Vasco® OP-Sensitive.42, 43 Gloves should not be donned until hands are completely dry after hand disinfection, as this increases the risk of perforations and promotes more skin irritation. The frequency of glove perforation during surgery is between 12.7 and 31 percent. When using two gloves on top of each other (double-gloving), the risk of perforation of the inner glove is 3.8 to 13 percent.44-46
In general, surgical gloves should be changed every 60 minutes. Gloves should also be changed before inserting an implant45 and, of course, also after completion of the “non-clean part” of an operation (e.g., after bowel resection).
There are three different ways to put on gloves. A distinction is made between ‘closed’, ‘open’ and ‘assisted’. The open method should not be used for surgical procedures. The safest method is the assisted method, as contamination has also been detected in 100 percent of cases47 where the closed method is used. This particular one focused on the cuff area.47
Fingernails and jewelry: Fingernails should be cut short and finish at the fingertip.48 Wearing artificial nails has been associated with multiple nosocomial hospital outbreaks and must therefore be forbidden in the operating room.49-51 Jewelry (including wedding rings) should also be avoided due to the increased risk of perforation of surgical gloves.52
The time of antibiotic administration should be 60-120 minutes prior to the incision53, 60 so that a maximum activity level is reached and should be repeated every 90-120 minutes wherever necessary.
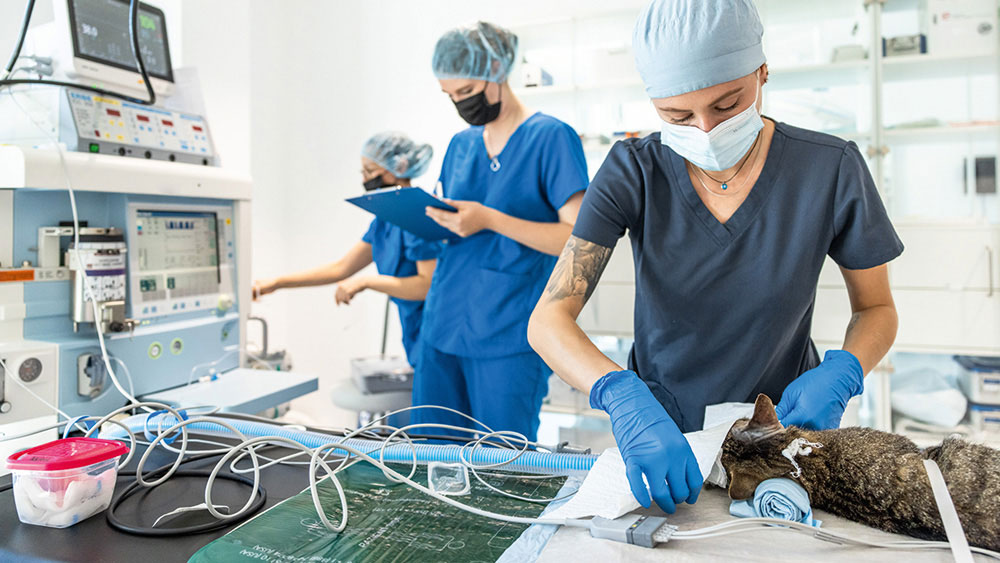
Duration of the operation: The operation time should be kept as short as possible2, 4, 53 as the risk of an SSI from the 70th to the 90th minute doubles3, 19 and from the 120th minute is sixfold compared to a 60 or 30-minute operation.53
Surgical technique: In general, a gentle surgical technique and atraumatic treatment of the tissue are considered important prerequisites for good wound healing.20
Aseptic irrigation prior to wound closure: Aseptic irrigation prior to wound closure leads to a significant reduction in the SSI rate in human medicine.20 Therefore, irrigation of the wound prior to closure with polyhexanide solution (e.g., Lavasurge®) is recommended.
Wound closure: The wound should be closed with the finest possible suture material. A wound cover with polyhexanide gel (e.g., Prontovet® Gel) is advantageous.20
Instrumentation: The instruments must be sterile. High technical quality contributes to a shortening of the operating time and a more atraumatic tissue treatment. The sterile instruments must first be covered or provided immediately before the operation, as otherwise they may be contaminated by contact or by staff members’ skin flakes and microflora suspended in the ambient air.56, 57
Number of people: Lots of movement and conversations during an operation go hand in hand with an increased SSI risk. The number of people should therefore be kept as low as possible and doors should remain closed as far as is possible.58, 59